FHO+: Continuity of care measure explained
Understand how continuity of care is measured and learn about the value, timing and real-life scenarios behind capitation adjustments in this new video series.
This video explains how the Continuity of Care is measured and evaluated. It reviews:
- What the measure counts: Visits for in-basket services made by your rostered patients to family physicians (OHIP specialty ‘00’)
- The list of acceptable physicians that count towards your measure
- The threshold is 75 per cent for each quarter
Within a quarter, 75 per cent or more of visits for in-basket services should be to you, another physician in your FHO group, or to an acceptable physician.
This video explains when and how you will be notified by the ministry regarding your Continuity of Care measure.
You will:
- Receive a monthly report of your roster’s continuity of care measure, based on the available claims data for the previous month
- Continue to receive your Outside Use reports
The notification provides you with an opportunity to course correct, similarly to how you would with Negation.
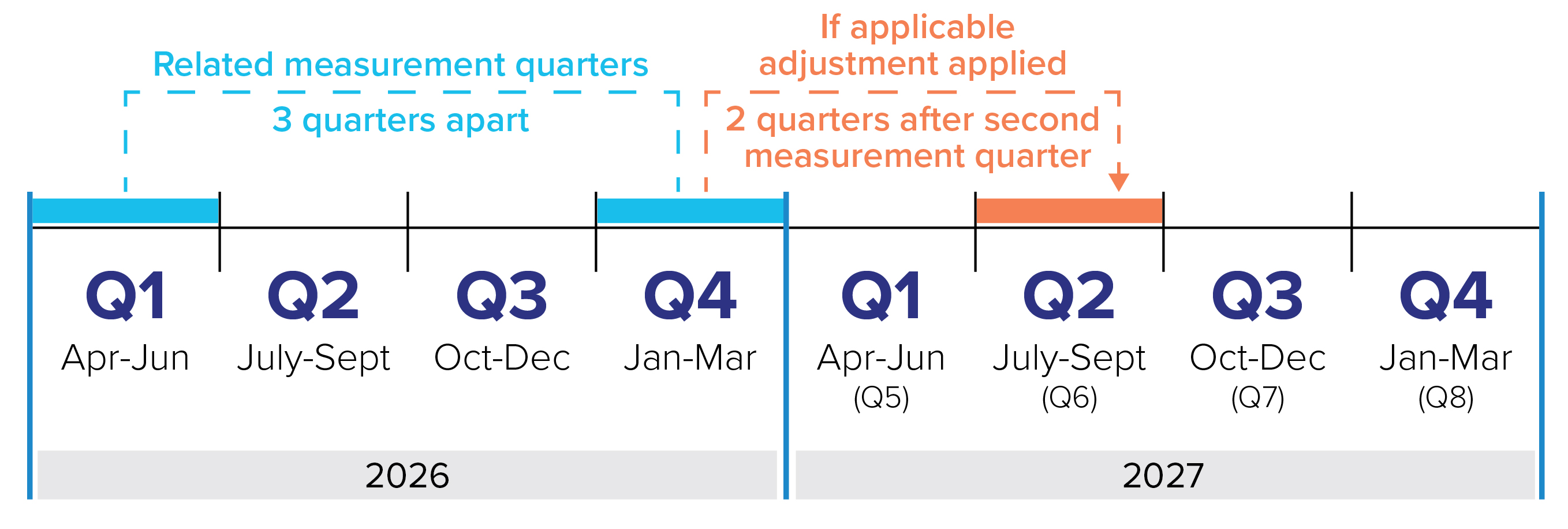
This video explains what triggers a capitation payment adjustment. It illustrates the following concepts:
- Related measurement quarters are three quarters apart
- Both related measurement quarters must be below the 75 per cent threshold for a capitation payment adjustment to apply
This process resets every quarter and continues on a rolling basis.
A single quarter below the 75 per cent threshold is not a reason to worry. It’s a nudge for you to review your roster’s activities and look for ways to improve.
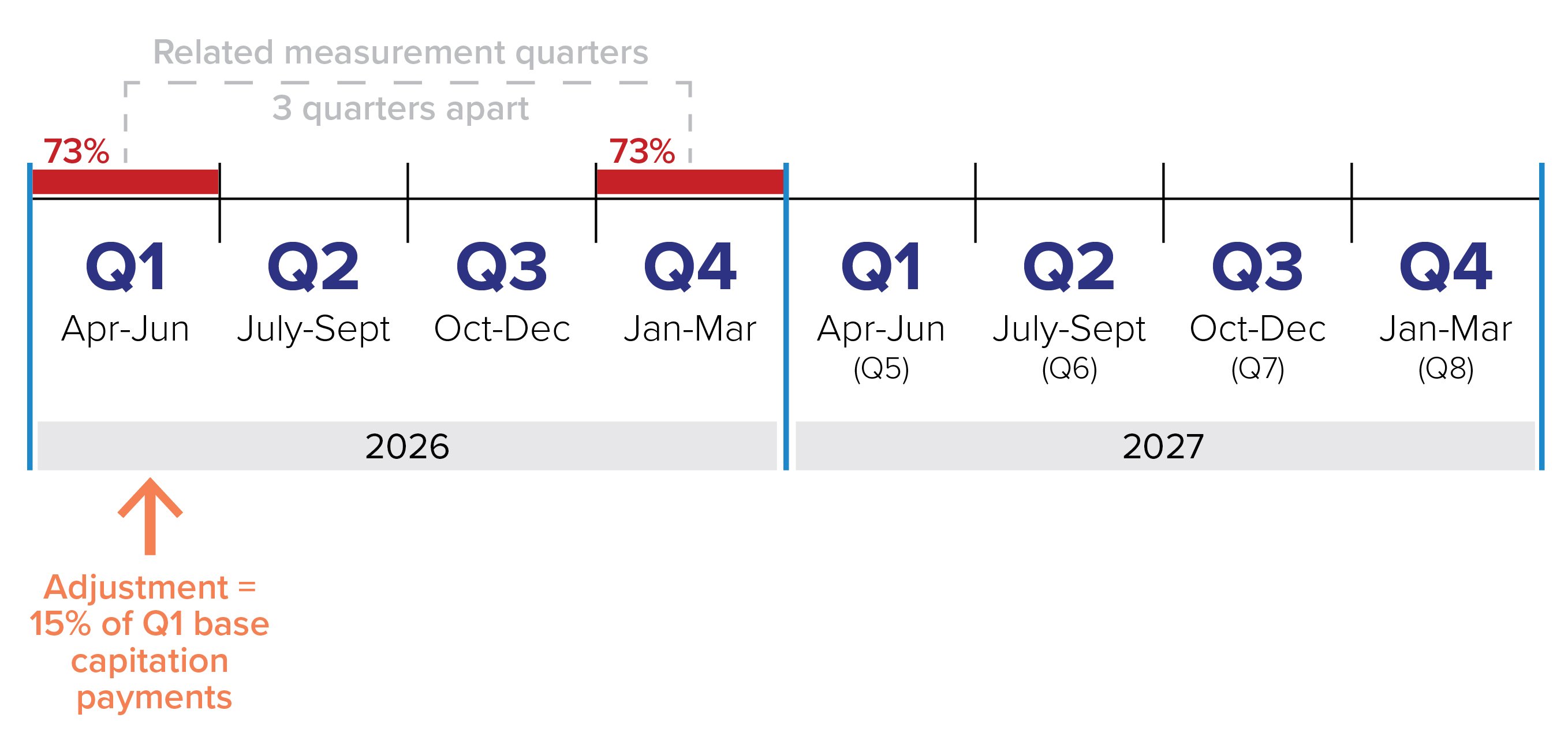
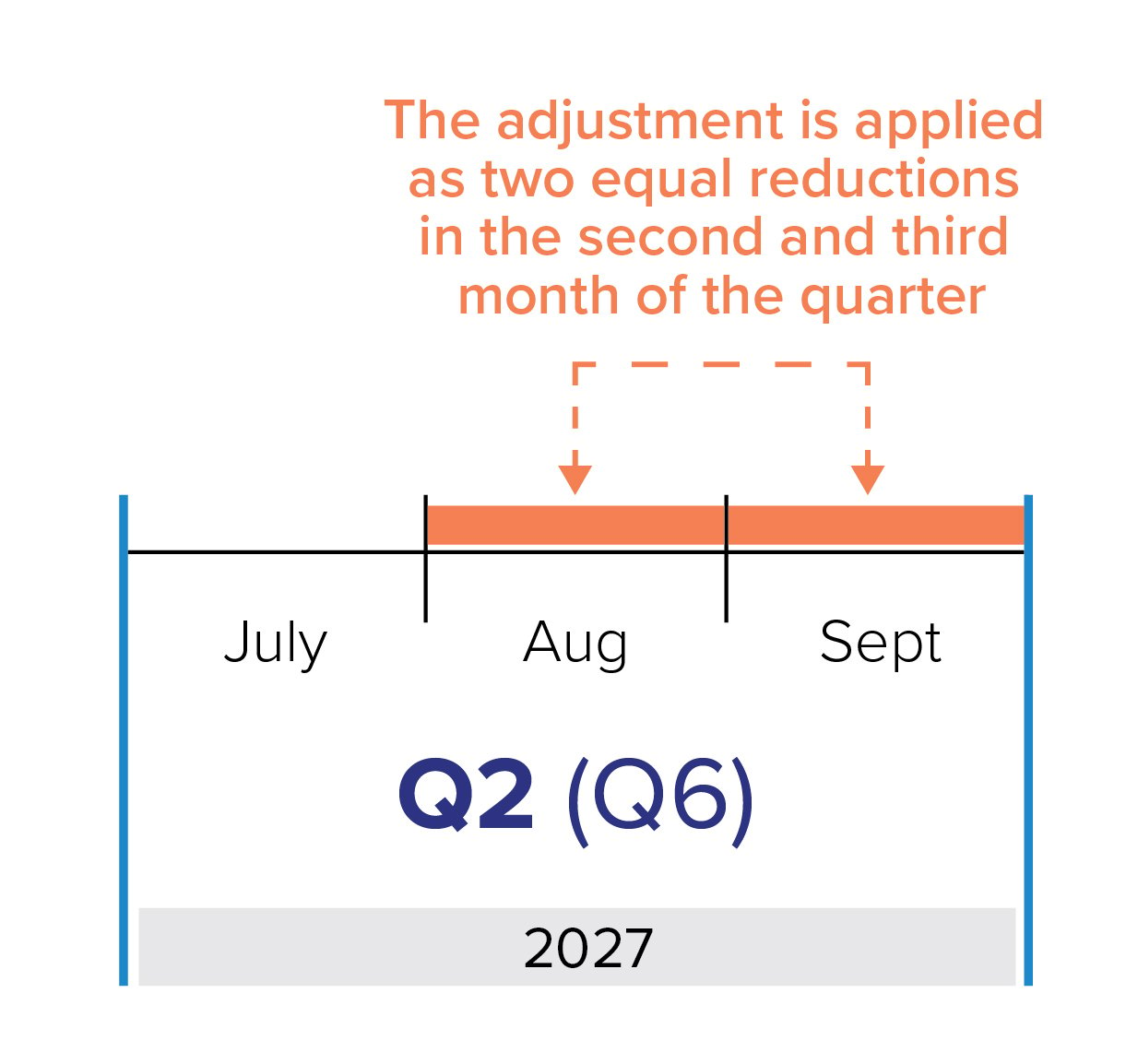
This video shows how a capitation payment adjustment is calculated and when it is applied. It illustrates the following concepts:
- Both related measurement quarters must be below the 75 pre cent threshold for a capitation payment adjustment to apply
- If these conditions are met, a capitation payment adjustment will be made two quarters after the second related measurement quarter
- The value of the adjustment is 15 per cent of the value of the base capitation payments made to you in the first of the two related measurement quarters
Facing a capitation payment adjustment in one particular quarter doesn’t mean that you’ll continue to face a penalty every quarter after that.
The process starts again every quarter, looking only at the two related measurement quarters.
Scenarios
This video is a case example of a physician who has a single quarter where their Continuity of Care measure is below the 75 per cent threshold. They do not face a capitation payment adjustment.
It illustrates the concept that an adjustment only applies if both related measurement quarters are under 75 per cent.
This video is a case example of a physician whose Continuity of Care measure is below 75 per cent for two related measurement quarters. She is subject to a capitation payment adjustment as a result.
She uses the information available to make adjustments to her practice and return to full capitation payments.
It illustrates the concept that financial consequences are temporary if the physician’s Continuity of Care measure improves.
Step by step: understanding the potential financial consequences
The continuity of care measure for each FHO physician is calculated quarterly and evaluated on a rolling basis. If your roster’s continuity of care is below the 75 per cent threshold for both related measurement quarters, an adjustment will be applied to a future quarter. The adjustment is calculated on the value of base capitation payments, excluding acuity payments.
Interactive calculator
To experiment with how this will work in practice, access the OMA’s Continuity of care calculator/worksheet