FHO+ is the future of family medicine
On April 1, 2026, family medicine is changing for the better. Existing FHOs will transition to the new FHO+ model after signing the updated FHO contract by March 31, 2026.
FHO+ addresses the issues that family doctors have told us about time and time again, including administrative burden, increasing complexity and lagging compensation.
The goal: Bring back the joy of family medicine, and build a foundation to support recruitment and retention.
We worked closely with the Section on General and Family Practice each step of the way, while incorporating best practices from other jurisdictions.
Tools and resources to help you make the transition to FHO+
Billing changes
- A recording from the FHO+ billing changes webinar held on March 11 (member-only access)
FHO+ compensation
Hourly rate
- Hourly rate guide (fee codes now available)
- Printable reference sheet
- Eligible hours calculator
- EMR recommendations and resources
- Hourly rate FAQs
Continuity of care accountability
- Continuity of care guide
- Continuity of care FAQs
- Continuity of care payment adjustment calculator
- Continuity of care measure explainer videos
Patient attachment bonuses*
- Patient attachment bonuses guide (member-only access)
- Patient attachment bonuses FAQs
Agreements and forms
- Agreements and forms guide, including updated FHO contract (member-only access)
- OMA Learns course: Understanding the FHO+ contract (member-only access)
Other resources
*Patient attachment bonuses will be available in all patient enrolment models
Patient attachment bonuses
Learn about patient attachment bonuses available to family physicians in all patient enrolment models.
Compensation model
Funding FHO+
Payment calculator
Physician scenarios
CoC accountability
Compensation model
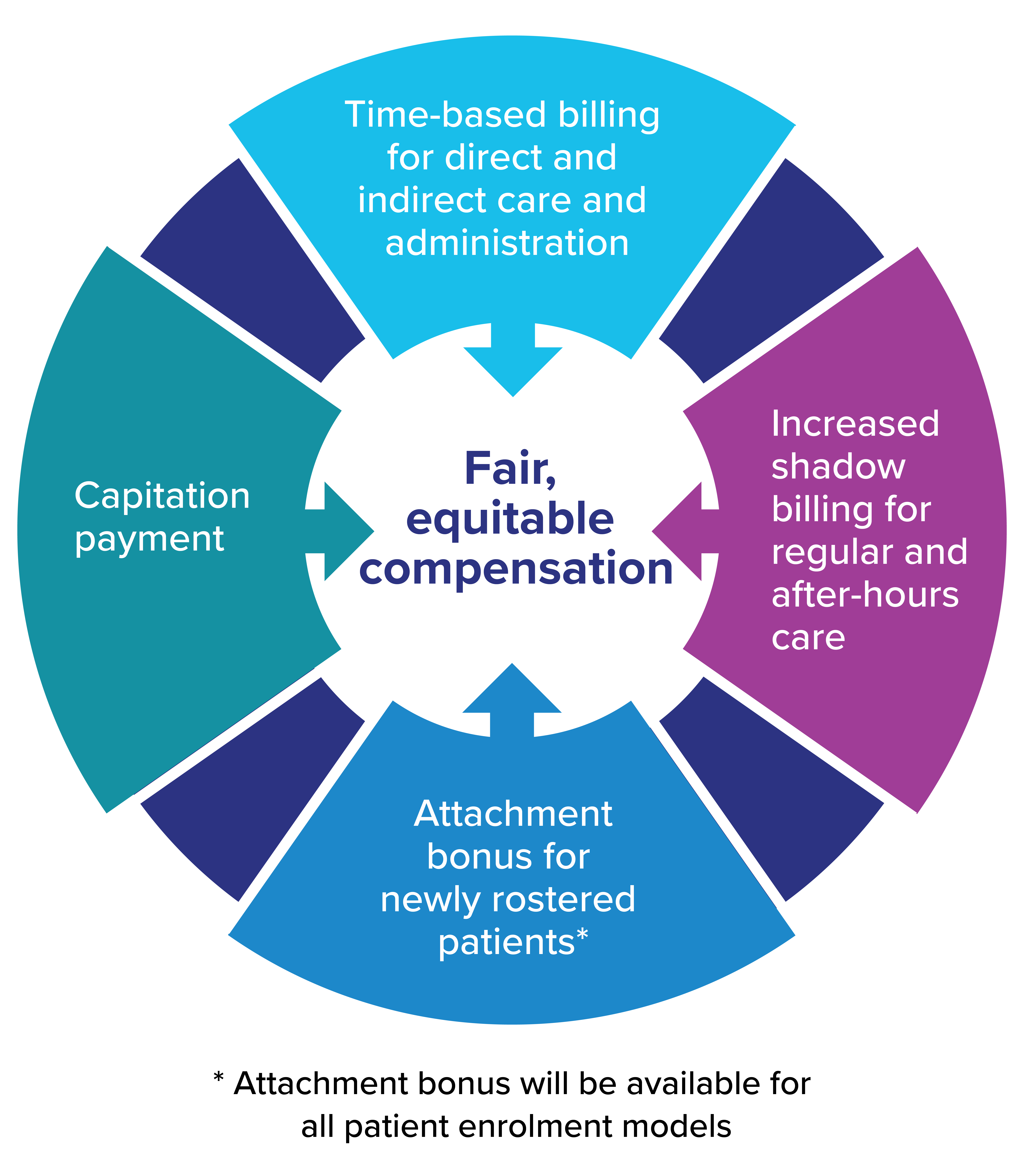 The most important improvement under FHO+ is time-based billing that pays an hourly rate for all direct and indirect care.
The most important improvement under FHO+ is time-based billing that pays an hourly rate for all direct and indirect care.
The benefits are transformative. Under FHO:
- You are paid for clinical administrative work
- You are paid for indirect care, such as reviewing lab results
- You are compensated for the time you spend on clinical teaching, when supporting patients
- When you spend more time on a more complex patient, you are compensated for it
Under FHO+, capitation payments remain the same, and there will be significant increases to shadow billing and the after-hours premium.
Physicians will also receive a bonus for rostering unattached patients, with a higher bonus in remote areas or when the patient is older or more complex.
The attachment bonus will also be available for family physicians in other patient enrolment models. Learn more about the patient attachment bonuses (member-only access).
Time-based billing
There are three types of work that you can bill under the hourly rate: direct patient care, indirect patient care, and clinical administration.
The hourly rate pays $80, with one exception. Telephone-based virtual care pays $68 per hour when the physician is not present in their clinic to deliver the service. All virtual care delivered from the clinic is paid the full $80, as is video-based virtual care provided off-site.
Guide to the hourly rate
Want to learn more? Check out our new guide for information on billing codes, limitations and more.
Shadow billing
Shadow billing will increase substantially. For most in-basket services, shadow billing will rise from 19.4 per cent to 30 per cent. We also negotiated a higher 50 per cent shadow billing rate for the in-basket procedures listed below to encourage physicians to provide these services and to compensate for procedures that have higher associated costs.
After-hours premium
The after-hours premium will increase from 30 to 50 per cent. The existing requirements for after-hours care will remain in place.
Enhanced Group Management Leadership Payment
FHOs are eligible for a group management leadership payment of $1 per enrolled patient each year, up to a maximum of $25,000. Under FHO+, there is an additional Enhanced Group Management Leadership Payment that supplements the existing GMLP.
The enhanced payment pays $4 per patient each year, up to a limit of $100,000 per group. This is intended to compensate leads for ensuring compliance with the FHO contract, such as requirements for after-hours availability and care.
Together, that’s a maximum payment of $125,000. FHO+ also introduced a combined minimum payment of $25,000.
In-hospital services
Under FHO+, in-hospital services are considered out-of-basket, they won’t impact the FFS limit and they're paid the full fee-for-service rate. This enhancement will also be available under the FHN model.
Under the original FHO model, inpatient hospital services were paid via shadow billing.
Funding FHO+
We obtained significant new funding for FHO+. Because the hourly rate represents a very large investment, we supplemented new funding with the funding that was previously used for the CCM fee and access bonus.
However, a typical FHO physician only needs to work just under 12 hours per week (working 46 weeks per year) to match what they’re currently receiving from the CCM fee and access bonus.
For the vast majority of FHO physicians, this will be a clear benefit.
More compensation for existing FHO doctors
Throughout the development of FHO+, we modelled how the new structure would impact existing FHO physicians. Our latest analysis shows that the vast majority of FHO doctors will receive a significant increase in compensation under FHO+.
Scenarios
See below for three scenarios for physicians with varying roster sizes.
We have estimated the amount of time that an average doctor would bill, since we don’t currently collect that data. If you work more hours than our estimate, you will earn more compensation.
Dr. A’s current practice has an average roster size of 660, with 1,687 total enrolled visits to this group. Dr. A works an average of 205 days per year, with 2.6 visits per year per rostered patient and 36.7 visits per week. Dr. A works 15.3 hours per week.
| Current remuneration breakdown | New payments (hourly @ $80) | |
| Base | $114,901 | $114,901 |
| Shadow | $10,915 | $16,590 |
| FFS | $65,216 | $71,411 |
| Other income | $15,078 | $15,078 |
| Access bonus* | $12,838 | $0 |
| CCM | $23,249 | $0 |
| Hourly rate | $56,244 | |
| Other targeted | $7,500 | |
| TOTAL | $242,196 | $281,725 |
| % difference | 16% |
*real access bonus dollars
Dr. B’s current practice has an average roster size of 1,220, with 2,837 total enrolled visits to this group. Dr. B works an average of 234 days per year, with 2.3 visits per rostered patients per year and 61.7 visits per week. Dr. B works 25.7 hours per week.
| Current remuneration breakdown | New payments (hourly @ $80) | |
| Base | $213,392 | $213,392 |
| Shadow | $18,530 | $28,166 |
| FFS | $72,067 | $78,913 |
| Other income | $16,213 | $16,213 |
| Access bonus* | $25,041 | $0 |
| CCM | $43,818 | $0 |
| Hourly rate | $94,567 | |
| Other targeted | $7,500 | |
| TOTAL | $389,062 | $438,751 |
| % difference | 13% |
*real access bonus dollars
Dr. C’s current practice has an average roster size of 2,373, with 5,415 total enrolled visits to this group. Dr. C works an average of 265 days per year, with 2.3 visits per rostered patient per year and 117.7 visits per week. Dr. C works 54.3** hours per week (**capped for illustrative purposes).
| Current remuneration breakdown | New payments (hourly @ $80) | |
| Base | $405,889 | $405,889 |
| Shadow | $30,596 | $46,505 |
| FFS | $133,263 | $145,922 |
| Other income | $15,726 | $15,726 |
| Access bonus* | $42,793 | $0 |
| CCM | $85,129 | $0 |
| Hourly rate | $180,505 | |
| Other targeted | $7,500 | |
| TOTAL | $713,395 | $802,048 |
| % difference | 12% |
*real access bonus dollars
Notes:
- Estimated hours worked in each scenario are based on the best available data, incorporating reported averages for administrative responsibilities
- Unless otherwise specified, each visit is assumed to require 25 minutes of physician time
- Scenarios are calculated based on the assumption that physicians typically work 46 weeks per year
Payment calculator
You can use this calculator to estimate what changes you may experience with this model.
To find these numbers on your RA, search for the following bracketed terms. You can find these on the Payment Summary Report page of the solo RA report.
- Capitation payment (“Base Rate payment”)
- Access bonus payment (“Access Bonus”)
- CCM payment (“Comprehensive Care Capitation payment”)
- Shadow billings (“Blended Fee-For-Service premium”)
See an example of where to find these terms on a sample RA report.
Please enter monthly amounts from your RA
| Payment Type | Monthly Amount ($) |
|---|---|
| Capitation Payment | |
| Access Bonus Payment | |
| CCM Payment | |
| Shadow Billings |
Please enter your roster and hours
| Item | |
|---|---|
| Roster size (number of patients) | |
| Weeks worked per year |
| Hours worked per week: | |
|---|---|
| a) Direct Care: in-person and virtual (with the exception of ‘b’) | |
| b) Direct Care: care provided by telephone when MD not in office | |
| c) Indirect Care | |
| d) Clinical Admin | |
| Total hours eligible for hourly rate | 0 |
Your expected change in income
| Current Annual Income | |
| New Annual Income | |
| Capitation Payment | |
| Shadow Billings | |
| Hourly Payment | |
| Change ($) | |
| Change (%) |
* No more than 25% of the total physician’s hours billed (averaged over 28 consecutive days) can be for indirect patient care and clinical administrative work. Clinical administration time (CAT) will be no more than 5 percent of the total amount of time claimed by the physician for direct and indirect patient care, measured over twenty-eight consecutive days.
NOTE: This calculator is provided as illustration only and as a rough estimate of what changes physicians may experience.
Creating a new FHO
When consulting with physician leaders, we heard that family doctors often face unnecessary barriers to forming a FHO. Co-location guidelines present a significant challenge, especially in remote areas of the province. Under FHO+, these guidelines will be significantly relaxed for remote regions.
Managed entry limits will also be increased retroactively for Year 1 of the PSA, with the unused allotment rolling over into future years. Physicians currently in an FHG will no longer be subject to managed entry limits, however, it is important to keep in mind that co-location guidelines will apply to all physicians as they do now, including those in a FHG.
Here’s how things will change:
| FHO | FHO+ | |
| Minimum physicians in the FHO | 6 | 6 |
| Minimum physicians at each location | 3 | 2 |
| Maximum distance between locations (definition of “close proximity” as per FHO agreement) |
Five kilometres. If RIO is more than one, consideration may be given |
Varies based on RIO score: Zero: five km One to five: 10 km More than five: 30 km |
| Dispute resolution mechanism | PSC co-chairs | PSC co-chairs and referee |
| Total managed entry allotment (unused allotment rolls over into future years) | Forty physicians per month | Sixty physicians per month for first year of PSA, future years to be determined |
| Managed entry for FHG physicians | Subject to managed entry limits | Not subject to managed entry limits |
We know that co-location and managed entry are just one piece of the puzzle. The current process for forming a FHO can be lengthy, stressful and daunting. We are advocating for a streamlined process that is more straightforward and less time-consuming.
Continuity of care accountability metric
FHO+ includes a continuity of care accountability metric for patient access. This is calculated by determining the percentage of in-basket visits that are provided to your rostered patients by you, a physician in your FHO or another acceptable provider such as a focused practice physician. The Board of Arbitration set a benchmark of 75 per cent (member-only access).
Throughout the negotiation and arbitration process, we worked to build a model with built-in incentives that will encourage FHO physicians to provide reliable and consistent access for their patients. The ministry pushed for an accountability we felt was unnecessary, and we worked to minimize any impact on physicians.
All FHO physicians will receive continuity of care reporting, and any physicians that fall below 75 per cent will have an opportunity to improve their metric without facing any penalty. The Board of Arbitration has set the penalty at 15 per cent of the capitation payment.
We want to help you understand how the ministry will calculate and report your continuity of care. Visit our new continuity of care page to learn more.